There are extensive recommendations from the American Academy of Orthopaedic Surgeons about Management of Rotator Cuff Injuries Clinical Practice Guidelines, Published in March 2019. Some strong and moderate recommendations are listed below. Weaker recommendations have not been listed.
STRONG = Evidence from two or more “High” quality studies with consistent findings for recommending for or against the intervention.
MODERATE = Evidence from two or more “Moderate” quality studies with consistent findings, or evidence from a single “High” quality study for recommending for or against the intervention.

Management of small to medium tears
Strong evidence supports that both physical therapy and operative treatment result in significant improvement in patient-reported outcomes for patients with symptomatic small to medium full-thickness rotator cuff tears.
Management of large tears
Surgery for rotator cuff tears
Moderate evidence supports that [surgically] healed rotator cuff repairs show improved patient reported and functional outcomes compared to physical therapy and unhealed rotator cuff repairs.
Non-surgical Management
Strong evidence supports that patient reported outcomes (PRO) improve with physical therapy in symptomatic patients with full thickness rotator cuff tears. However, the rotator cuff tear size, muscle atrophy, and fatty infiltration may progress over 5 to 10 years with non operative management.
Imaging
Strong evidence supports that MRI, MRA, and ultrasound are useful adjuncts to a clinical exam for identifying rotator cuff tears.
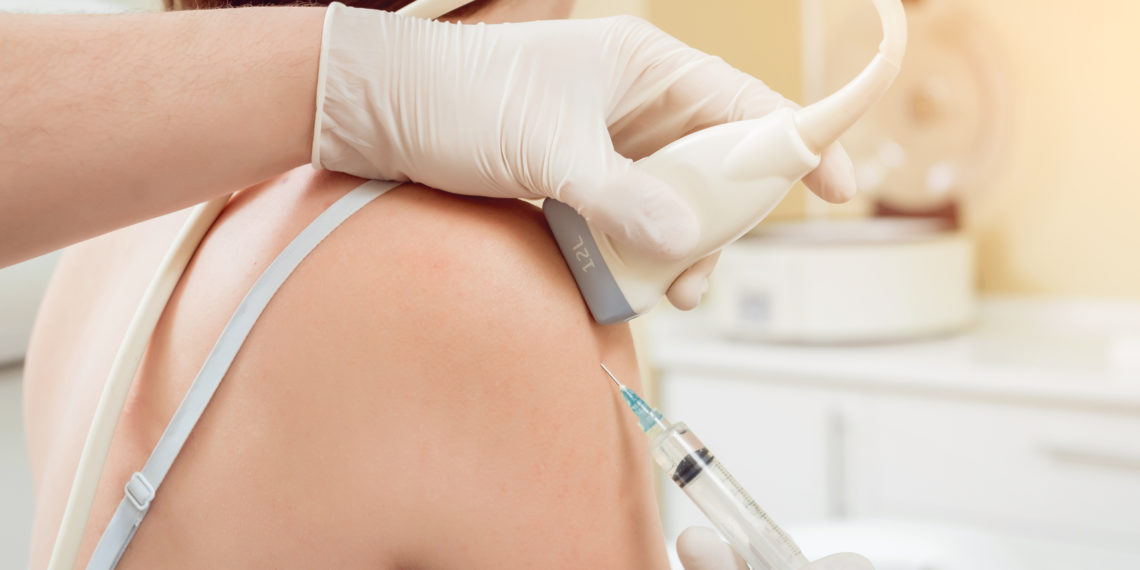
Corticosteroid Injections
Moderate evidence supports the use of a single injection of corticosteroids with local anesthetic for short-term improvement in both pain and function for patients with shoulder pain.
Higher grade Partial Thickness Tears
Strong evidence supports the use of either conversion to full-thickness or transtendinous/in-situ repair in patients that failed conservative management with high-grade partial-thickness rotator cuff tears.
Other Factors
Strong evidence supports that older age is associated with higher failure rates and poorer patient reported outcomes after rotator cuff repair.
Moderate evidence suggests that patients with diabetes will have higher re-tear rates and poorer quality of life and patient reported outcome scores after rotator cuff repair.
Strong evidence supports no difference between OPEN and ARTHROSCOPIC REPAIR
Strong evidence supports no difference in long-term (> 1 year) patient-reported outcomes or cuff healing rates between open and arthroscopic repairs; however, arthroscopic-only technique is associated with better short-term improvement in post operative recovery of motion and decreased visual analog score (VAS) scores.
