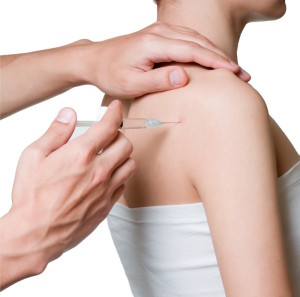
CORTICOSTEROID INJECTIONS FREQUENTLY ASKED QUESTIONS
Iain has also co-authored a comprehensive corticosteroid injection consumer guide with additional information for health professionals in Inside Radiology a project of The Royal Australian and New Zealand College of Radiologists. Here are the links to the Inside Radiology guide to Bursal Injections and Carpal Tunnel Injections.
WHY HAVE I BEEN REFERRED FOR AN ULTRASOUND GUIDED STEROID INJECTION?
The commonest cause of joint pain is arthritis. Though there are many causes of arthritis most of them are associated with some form of joint inflammation or synovitis. A common cause of soft tissue pain is bursitis and tendinopathy. A bursa is a soft tissue space between two structures such as bone, muscle and tendon. It is like a “soft tissue” joint.
A bursal or joint injection is generally undertaken to reduce any inflammation in joints (SYNOVITIS), bursa (BURSITIS) or around tendons (TENDINOPATHY) . By injecting small doses of corticosteroid and/or local anaesthetic medication directly into these structures any pain arising from the site should be relieved. This pain relief and swelling reduction will help the function of the soft tissues on either side of the joint or bursa, which in turn can physiotherapy treatments more effective. To make sure the injection goes into the joint or bursa itself where it has the best chance of working, the needle for the injection is usually guided by imaging, most often using ultrasound.
ARE THERE OTHER REASONS WHY HAVE I MIGHT HAVE BEEN REFERRED FOR AN ULTRASOUND GUIDED STEROID INJECTION?
Sometimes it can be difficult for your doctor to know exactly what is causing your pain. If the pain is not due to bursitis or from the adjacent tissues the injection may not improve your symptoms. Although this may be disappointing to you, it can be helpful information for your doctor as it means that other possible causes need to be investigated.
HOW DO I PREPARE FOR A STEROID INJECTION?
No specific preparation is needed. If the injection is in the foot, hand or arms you may need a driver afterwards. Please bring any previous X-rays, ultrasound, CT or MRI scans taken as part of your assessment for this problem. Please wear comfortable clothing with easy access to area being injected.
WHAT HAPPENS DURING A ULTRASOUND GUIDED STEROID INJECTION?
You will be placed in comfortable position (on a scanning bed usually). A staff member and/or the doctor will explain the procedure to you. You will be able to ask any questions. Then the area to be injected is scanned and the skin cleaned. Sometimes a mark on the skin is placed by the doctor to help guide the needle entry. A narrow bore needle is then passed from the skin directly into the joint or bursa while being scanned (usually with ultrasound) to help guide the doctor to place the needle in a precise location. A small volume of fluid (usually just a few millilitres) is then injected and the needle withdrawn. The needle is generally in and out again with a minute. Local anaesthetic is used and the commonest substance injected is celestone chronodose. Most patients are surprised at how quick and easy the procedure is.
ARE THERE ANY AFTER EFFECTS OF A STEROID INJECTION?
Like any injection there is sometimes a dull ache for a few hours following the procedure. There is often a zone of local numbness related to the local anaesthetic for one or two hours. Local bruising and bleeding at the site of the needle can occasionally occur. The affected limb or part should generally be rested completely for 6 hours, and then minimise use of the part for between 1 and 3 days, sometimes longer. You will be advised what is best for you by the doctor. The corticosteroid doesn’t start working usually for 24hrs and sometimes up to 3 days. During this time the normal symptoms may continue or occasionally are worse. A major flare of symptoms generally indicates a local reaction is occurring to a part of the injected material or simply to the needling. If the reaction is distressing then you should contact your own doctor or the clinic where you had the procedure.
HOW LONG DOES A STEROID INJECTION TAKE?
The injection procedure itself rarely takes more than five minutes but the preparation (scanning, marking, cleaning the skin,etc) is important and will take approximately 15 minutes. Sometimes your doctor has requested a full scan and/or assessment before the procedure usually to locate and/or confirm the target or problem. This will be time in addition to the procedure. You may be asked to rest or wait for a short time after the procedure.
WHAT ARE THE BENEFITS OF A STEROID INJECTION?
The aim is primarily to reduce any inflammation in or around the targeted structure. By injecting small doses of corticosteroid and/or local anaesthetic medication directly into the bursa any pain arising from it should be relieved. This pain relief and swelling reduction will help the function of the soft tissues on either side of the joint or bursa, which in turn can physiotherapy treatments more effective. Sometimes the procedure is undertaken for diagnostic reasons. Your doctor may be uncertain about the origin of your pain and wishes to undertake the procedure to help identify the source of the pain. As the effect of the injections is quite localised a good response to injection confirms the source of pain whereas a lack of response (no improvement in symptoms) indicates the pain is not arising from the bursa or its adjacent structures. The relief of symptoms is variable in duration –it might last a few weeks or several months. It is therefore only part of an overall management plan for you.
WHAT ARE THE RISKS OF A STEROID INJECTION?
This is a very safe procedure with few significant risks. Few patients complain of side effects but occasionally problems are experienced. The commonest complaint is a temporary aggravation of the symptoms over one, two, or even three days. Very rarely patients get general symptoms related to absorption of the corticosteroid into the circulation. This generally only occurs either when larger doses are used or in some patients who are more sensitive to corticosteroids. In diabetics this absorption can increase the blood sugar levels –which should generally be checked several hours after the procedure.There is a risk of local damage to the soft tissues at the injection site. Tissue atrophy (a thinning or weakening) of the skin or subcutaneous fat (found just beneath the skin) rarely occurs when the injected material is very close to the surface. Tissue atrophy can also involve deeper structures. It is more likely with repeated injections at the same location. Some patients find that the injection gives them pain relief for a few months, but then the pain comes back and they wonder about the safety of having another injection. Although the exact risk of multiple injections is not known, most doctors would advise against injection more than 3-4 times a year to avoid tissue atrophy. This is more important when the injection is being done in areas in which there is already significant wear or tear (torn tendons or ligaments). extremely rarely people are allergic to the injected medication (as with any drug). The exact risk of this is not known. There is a risk of infection, which is very small and probably lies between 1 in 20,000 and 1 in 75,000 injections performed. The procedure should not be performed if there is broken skin or infection overlying the bursa, or if the bursa may already be infected. Recent studies show steroid injections should probably not be given within 3 months of a planned total joint replacement as there is a slightly higher risk of postoperative infection of the prosthesis.
For more information on corticosteroid injections search the site.
For a video showing an ultrasound imaging of a guided steroid injection GTB Inject edited