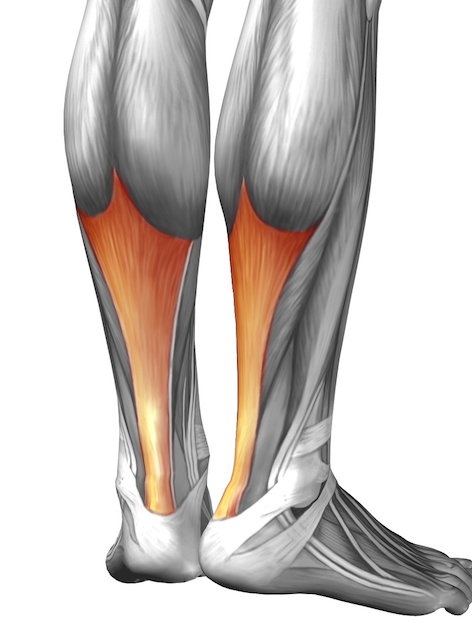
WHAT IS TENDINOPATHY?
Tendinopathy is a term used for painful conditions occurring in and around tendons in response to injury and/or overuse and ageing. The natural course of symptoms is variable but most ultimately resolve (even if the tendon appearance on scans does not). Generally the length of symptoms varies according to age and severity. A recent study suggested the median length of symptoms was 14 months. The incidence of symptoms in sedentary people is highest in middle age though at particular sites (lateral hips and shoulders) the incidence is greater with increasing age.
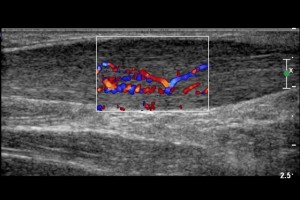
Achilles tendon swelling with micro-vascular change
HOW IS IT DIAGNOSED?
Ultrasound can confirm or rule out the diagnosis but the presence of tendinopathy on ultrasound does not necessarily indicate whether it is the cause of your symptoms. The relationship between symptoms and the scan findings is determined by a clinician who combines the clinical history, examination findings, and all test and scan results. The incidence of asymptomatic tendinopathy also increases with age (i.e. many patients have scan findings of tendinopathy but no real symptoms).
A (well performed) ultrasound or MRI scan will determine whether there are significant tendon tears, inflammation, bursitis, or other nearby soft tissue pathology. It can broadly categorise the type of tendinopathy which usually helps in determining treatment options.
[…]
READ MORE